Virtual care delivery presents with unique organizational, practitioner, and patient benefits and barriers that do not exist within traditional in-person care. Effective use of telehealth requires the provider to recognize whether or not a patient is appropriate for telehealth, communicate the advantages and disadvantages with the patient, and understand how to resolve technical issues. The goal of this course is to address these challenges and provide clinicians with best-practice strategies to effectively incorporate telehealth into their care delivery.
Telehealth: An Introduction to Virtual Care
Description
Chapters & Learning Objectives
1. Successfully Introducing Telehealth to Your Patients
In this section, we will cover how to determine if telehealth is right for your patient. To do this, we will look at the Evidence-Based Decision-Making model and discuss how our clinical expertise fits into this decision-making process. We will also go through best practices for introducing telehealth to your patients by breaking down the what, where, when, why, and how.

2. Navigating Patient Barriers to Telehealth With Shared Informed Decision Making
This section will break down the model of shared informed decision-making (SIDM) in patient communication. Through an example patient/therapist conversation, we look at how we can use the three different types of talk (team talk, option talk, and decision talk) to navigate patient barriers to receiving treatment through telehealth.

3. Blending Telehealth and In-Person Treatment for Optimal Outcomes
Figuring out how best to blend telehealth and in-person treatment should be considered on a case-by-case basis with each patient. In this section, we will look at four patient case examples, each with its own unique barriers and conditions. We will discuss how telehealth can be blended within the clinical care continuum in order to add value for your patients and improve overall care.

4. Telehealth Tech Tips for Success
Providing care through telehealth can mean having to navigate some technical challenges. In this section, we’ll go through best practices for hardware, software, and connectivity. We will also see how to troubleshoot technical challenges in real time with two different scenarios of a patient and therapist experiencing audio and video problems.

5. Visually Optimizing Your Telehealth Session
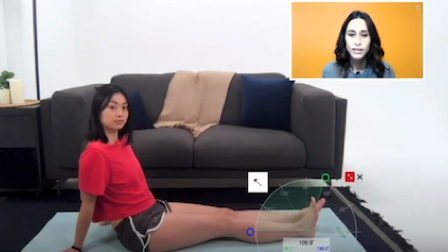
How you present yourself and frame your patient during a telehealth session can mean the difference between a positive or negative patient care experience. In this section, we will go through how to effectively present yourself to your patient, taking into account framing, lighting, environment, and clothing. We will also cover how to properly frame your patient to make sure you are able to successfully observe the patient’s movements during your session.

6. Translating In-Person Care to a Virtual Environment
Translating in-person care to the virtual environment means changing the way that we think about conducting an assessment and delivering treatment. In this section, we will cover best practices for coaching and cueing patient assessment techniques in a telehealth platform. We will also highlight the ways telehealth can be used to improve the patient treatment experience, virtually bringing the therapist into a patient’s home environment.

7. Building the Therapeutic Alliance During a Telehealth Visit
Building a therapeutic alliance with your patient is a key element in patient engagement and adherence to the therapy program. In a teleheath visit, building this alliance with your patient is more heavily weighted on communication skills compared to an in-person visit. In this section, we will cover how to build rapport with your patient in a virtual visit and discuss tips for motivational interviewing.